For people with kidney failure, the best treatment is often a kidney transplant. It has better survival and quality of life compared to dialysis. Now, new research suggests there is another important benefit.
“Transplantation is not only clinically advantageous—it is also the most resource-efficient and environmentally sustainable form of kidney replacement therapy,” says Dr. Christopher Nguan, a kidney transplant surgeon at Vancouver General Hospital and investigator with the Vancouver Coastal Health Research Institute.
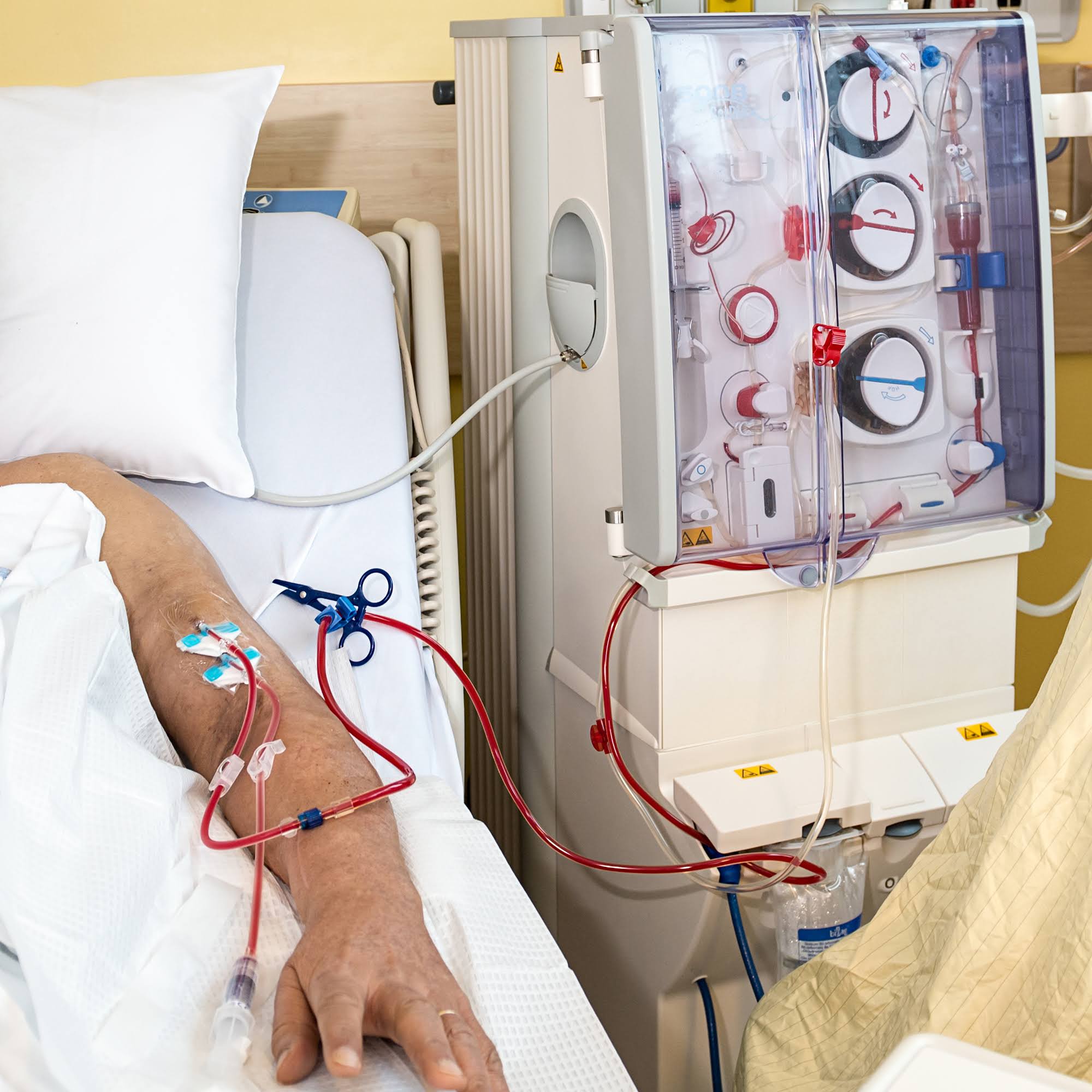
Comparing the environmental footprint of kidney care, Dr. Nguan and colleagues from the University of British Columbia’s Departments of Medicine and Surgery, along with UBC Okanagan’s School of Engineering, examined the environmental impact of three kidney replacement therapies (KRTs) — hemodialysis, peritoneal dialysis (done at home) and kidney transplantation. Their study, published earlier this year in the American Journal of Kidney Diseases, found that hemodialysis has a far higher climate impact than the other options. The emissions from a patient receiving hemodialysis was 74 per cent more than transplantation and 46 per cent more than peritoneal dialysis.
“What really stood out in our findings was the magnitude of the difference,” Dr. Nguan explains. “Hemodialysis was associated with several-fold higher emissions than transplantation, even when assessed over just one year of care.”
He adds that the long-term benefits of transplantation may be even greater, as transplanted kidneys can function for many years.
The research team examined a wide range of factors, including clinical processes, equipment use, energy consumption, transportation, laundry and waste. Data was drawn from provincial sources, energy audits and direct measurements. In addition to overall climate impact, they also looked at specific types of impact, such as air pollution, human toxicity and water depletion. Kidney transplantation had the lowest impact in all areas except terrestrial ecotoxicity due to the toxic immune suppression drugs required to prevent rejection.
The study also identified key contributors to environmental impact, travel and disposable single-use equipment.
“Modern healthcare, especially in the operating room, relies heavily on single-use materials, high energy consumption, and complex logistics. In kidney care, this is amplified—dialysis alone involves large volumes of water, plastics, and frequent patient transport multiple times per week,” Dr. Nguan remarks.
Dr. Nguan notes that modern healthcare systems were not originally designed with environmental considerations in mind.
“Everything we do is focused on maximizing patient safety and outcomes,” he comments. “But those same systems rely on energy-intensive processes and single-use materials.”
He hopes the findings will encourage healthcare planners to consider environmental impact alongside patient outcomes and cost when designing services.
The study points to several opportunities to reduce the environmental footprint of kidney care. These include expanding home-based therapies where appropriate, investing in transplantation programs and targeting high-impact areas such as transportation and medical consumables.
Such changes could have a meaningful impact. Chronic kidney disease affects an estimated 850 million people worldwide, with nearly four million people receiving some form of kidney replacement therapy.
Dr. Nguan and his team are now working to identify and test practical solutions that can reduce environmental impact without compromising patient care.
“I’ve coined the phrase ‘planet as our patient dyad’ to help frame how we move forward,” he says. “It reflects the idea that caring for patients and caring for the planet should go hand in hand.”
—--
Want to learn more about living donation? Please visit our website.